Online Enquiry Form
Overview
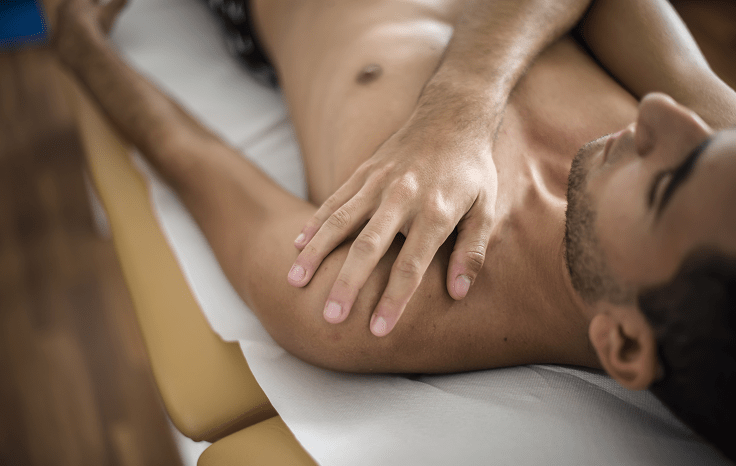
A rotator cuff tear is a very common muscle injury of the shoulder, commonly caused by sudden traumatic injuries, slow onset overuse injuries in those over 40’s, or degenerative changes in the shoulder joint in those over 50’s. The rotator cuff is a group of muscles that surround and protect the shoulder joint like a collar or “cuff” and provide multi-directional movement to the upper arm, allowing it to rotate, twist and turn. Rotator cuff tears are categorised by the thickness of the tear:
- Partial thickness tear.
- Full thickness tear.
They typically commence at the top of the shoulder and spread to the front or back of the shoulder as the severity of the condition worsens.
Symptoms
A rotator cuff tear can be painful and result in a dramatically reduced range of motion of the shoulder. Rotator cuff tear symptoms may include:
- Shoulder pain at the top and side of the shoulder.
- Weakness or loss of shoulder movement making it difficult to reach behind your back or reach upwards.
- Inflammation and swelling.

Causes
There are three causes of rotator cuff tear, namely sudden traumatic shoulder injury, repetitive overuse injury in those over 40’s and degenerative shoulder disease.
Sudden Traumatic Rotator Cuff Injuries
Sudden traumatic injuries of the rotator cuff happen when great or sudden forces cause it to over-stretch or forcefully tear. Falling on an outstretched arm or elbow can cause shoulder injury where the rotator cuff may be one of the structures damaged.
Repetitive Overuse Shoulder Injuries
From the age of 40 onwards, most people will begin to suffer muscle and tendon weakening. These changes mean people may no longer be able to generate force like they used to and overloading muscles may lead to tendonitis and tendon rupture. The rotator cuff tendon is susceptible to rupture as we age and we overload it with repetitive overuse activity like swimming, rowing, painting or plastering. The rotator cuff may experience repeated episodes of catching or impinging, which may progress to chronic impingement syndrome and ultimately rupture.
Degenerative Shoulder Disease
Degenerative disease of the shoulder affects those over 50’s and involves growth of bony spurs around the shoulder, joint disease and worsening blood supply. The effects of trauma and wear and tear are magnified and rotator cuff tear occurs more easily.
Diagnosis
To diagnose a rotator cuff tear, the consultant will question the patient to:
- Understand the nature of the injury (sports, work, accident, overuse etc).
- Determine the cause of the injury (impact, collision, fall, repetitive/slow onset).
- Understand the context of the suffering (age, return to sport, work, impact on daily living).
- Perform a physical examination to ascertain pain and range of movement.
- Perform specialised shoulder tests to confirm diagnosis.
Partial Thickness Rotator Cuff Tears
Partial rotator cuff tears are often painful and your arm may be weak or unable to be raised. Tests such as the empty can test are used to confirm suspected rotator cuff tear injuries.
Complete Thickness Rotator Cuff Tears
Complete rotator cuff tears are obvious as you will be unable to raise your arm at all. Additional movement tests such as reaching behind your back will determine the severity of your condition. Xray and MRI are used to uncover the presence of bony spurs, and the severity, size and location of the suspected injury.
Early diagnosis and treatment of rotator cuff tear injury is extremely important to avoid risk of a more complex injury.
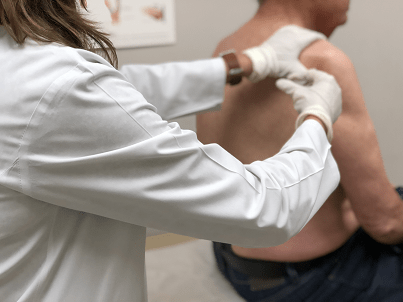
Treatment
Non-Surgical Treatment
Partial-thickness rotator cuff tear injuries may be treated non-surgically using:
- Rest.
- Pain and anti-inflammatory medication.
- Physiotherapy treatment for improved strength, better posture and function.
Surgical Treatment
Full-thickness rotator tears are indicated for surgery. The following methods are used:
Single Row Repair – Operation which repairs a small full-thickness tear.
Double Row Repair – Operation which repairs a large full-thickness tear.
Post Operative Rehabilitation
You will achieve the best surgical outcome if you follow up surgery with a matching course of rehabilitation. Following surgery, Dr Gupta will outline the most appropriate rehabilitation protocol for your physiotherapist to follow and communicate with your healthcare team to ensure that you receive the best post-operative treatment.
Please contact our friendly team on 02 9687 8344 or make an online enquiry here.

Dr Manish Gupta | MBBS FRACS FAOrthoA
Dr Manish Gupta is a renowned expert surgeon in the field of orthopaedic surgery specialising in upper limb including shoulder, elbow and wrist.